Arkansas Rep. Aaron Pilkington was reaching for a beer at a friend’s house when he saw something in the cooler he wasn’t expecting: plastic bags full of milk.
His friend’s wife explained that she was selling her extra breast milk to mothers who needed it for their babies. She couldn’t find a milk bank, so she resorted to posting it on Facebook Marketplace.
“I did some research and learned how much money Arkansas was sending out of state because the closest milk bank was in Texas,” Pilkington says. “In times of shortages, we were the last on the list to receive milk.”
Pilkington has sponsored legislation to increase access in his state to donated breast milk, a commodity even more in demand due to a shortage of infant formula. In 2021, the Human Milk Banking Association of North America dispensed 9.2 million ounces (roughly 72,000 gallons) of donor milk, a 22% increase from 2020.
With experts recommending exclusive breastfeeding for infants until at least 6 months, some states have looked to make donor milk more accessible through legislation. At least eight states passed bills in the last five years regulating and creating donor milk banks or requiring insurance coverage, both commercial and public, for donor milk under certain conditions.
Benefits of Exclusive Breast Milk
The short-term benefits of exclusive breastfeeding include reduced risks of ear infections and stomach bugs, and the long-term benefits include reduced risks of sudden infant death syndrome, asthma, obesity and Type 1 diabetes. Breast milk can be even more important for preterm infants who have an increased risk for necrotizing enterocolitis, a gastrointestinal disorder that causes inflammation of intestinal tissue, which can lead to serious illness and sometimes death. Breast milk has a protective effect against the disorder and promotes neurological development. The American Academy of Pediatrics recommends that very low birth weight infants be given donor milk when a mother’s milk is unavailable.
“It’s like liquid gold,” Pilkington (R) says. “It could be a lifesaver.”
Barriers to Access
But not all preterm and seriously ill infants in neonatal intensive care units have access to donor milk; not all hospitals prescribe donor milk or have it on-site. Hospitals bear the cost of storing, preparing and supplying the milk, even when the milk itself is covered by insurance. A handful of hospitals have their own milk banks, but these can cost up to $150,000 annually to maintain.
As with so many areas of society, those most in need are also among the most vulnerable, and for any product in a high-demand industry, costs run high. —New Jersey Assemblywoman Pamela Lampitt
Even if a hospital prescribes donor human milk, it is an expense that many cannot afford. The average cost is $3-$5 per ounce, and babies can consume between 32 and 48 ounces of milk per day. In states where neither Medicaid nor commercial insurance covers donor milk, families sometimes buy unregulated breast milk online or receive donated milk from friends or family because it can be less expensive. In both cases, there is a risk of transmitting diseases or exposing infants to prescription and illegal drugs; the FDA warns against buying breast milk from unregulated banks or online marketplaces.
“When we introduced this bill, mothers in need were turning to the internet to find affordable breast milk. Without regulation, those mothers had no way of knowing if that milk was safe,” says New Jersey Assemblywoman Pamela Lampitt (D), who sponsored legislation in her state to require insurance coverage for donor milk.
Barriers to donor milk disproportionately affect mothers insured by Medicaid, as well as Black infants and American Indian/Alaska Native infants due to their higher preterm birth rates. Even though these populations are the most likely to need donor milk, studies find that they are less likely to receive it at discharge from NICUs. The combination of higher rates of preterm births in Black and American Indian/Alaska Native communities combined with lower rates of receiving donor milk put these infants at increased risk for illness and death.
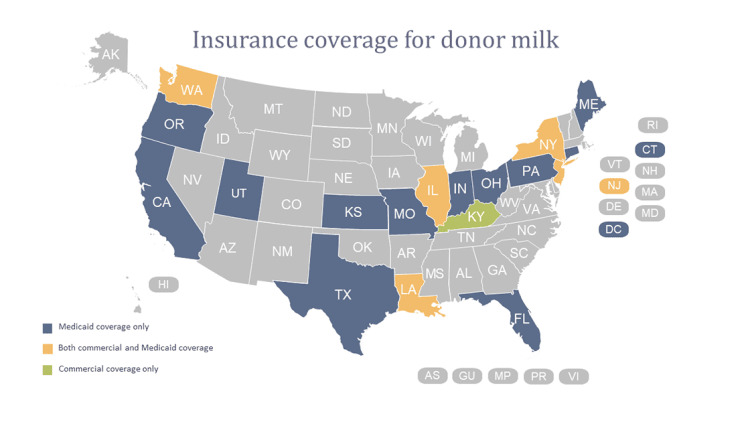
Data from Journal of Perinatology and NCSL Maternal and Child Health Database.
State Legislative Action
Coverage
States have increased access to donor milk by requiring insurance coverage, both public and commercial.
As of September, at least 17 states and the District of Columbia had enacted legislation requiring Medicaid coverage for donor milk; Indiana became the most recent state in August. Coverage varies based on the patients, length of time and settings. Coverage is required when donor milk is considered medically necessary, but state definitions vary. For example, Illinois requires an infant to meet one of seven medical requirements, ranging from low birth weight to hypoglycemia. Louisiana considers donor milk medically necessary when several criteria are met, including infant health, caregiver ability and source of donated milk.
State laws also differ in coverage period. Kansas covers up to three months of donor milk, New Jersey up to six months and Louisiana up to 12 months.
Some states require either inpatient or outpatient use, and others cover both settings. Florida stipulates that donor milk is covered only in the hospital setting;, Utah covers only outpatient donor milk; and New Jersey covers both inpatient and outpatient milk.
Illinois, Louisiana and New Jersey recently passed legislation requiring commercial insurance coverage for donor milk. These policies also vary in the patients and settings covered and may limit coverage to milk from accredited milk banks.
Milk Banks
In recent sessions, states also increased access to donor milk by creating or regulating milk banks. Pilkington sponsored legislation creating the Arkansas Milk Bank after learning that the state was buying milk from neighboring states. “During shortages, milk banks were prioritizing hospitals in their own states,” he says. “With the high preterm birth rate and the high rate of Medicaid-covered babies, we were sending thousands of dollars to other states.”
Now his state spends Medicaid dollars in state, and Arkansas mothers have a place to donate their milk. Pilkington believes this will be a step toward reducing the state’s infant mortality rate because of the nutritional benefits of breast milk, and he has hope that the increase in supply will prompt doctors to prescribe donor human milk.
Pennsylvania requires the state department of health to license milk banks and mandates that milk banks screen donors and pasteurize and test the milk. The law also creates licensing fees and prohibits the sale of human milk by unlicensed milk banks to ensure that donated milk is safe for infants.
States can statutorily regulate milk or promulgate rules and guidelines after legislation passes. For example, Maryland regulates donor milk as a human tissue, and Texas requires that human donor milk banks follow guidelines set by the state health department.
As states look to decrease disparities in infant mortality and infant health outcomes, increasing access to safe donor milk may be one lifesaving strategy for the most vulnerable infants. “As with so many areas of society, those most in need are also among the most vulnerable, and for any product in a high-demand industry, costs run high,” Lampitt says. “By requiring health benefits coverage, we ensured that any mothers facing challenges in feeding their infants have affordable access to breast milk, and the law now requires that the milk they receive meets the standards of quality both mother and child deserve.”
Kendall Speer is a policy associate in NCSL’s Health Program.