As EMS systems across the country continue to face challenges in workforce, funding and administration, providing timely and quality emergency medical services to all residents is a common priority. Several factors have long strained EMS systems, which were further stretched by the COVID-19 public health emergency. Challenges include the supply of EMS clinicians, limited funding, violence against EMS clinicians, long ambulance offload times and supply chain delays.
NCSL has maintained an EMS Legislative Database since December 2021, tracking enacted measures across all 50 states, select commonwealths and the territories.
State Actions
At least 39 states and territories enacted 113 bills in 2022 alone to address various aspects of EMS systems, including administration, funding, rules and regulations, systems of care and workforce.
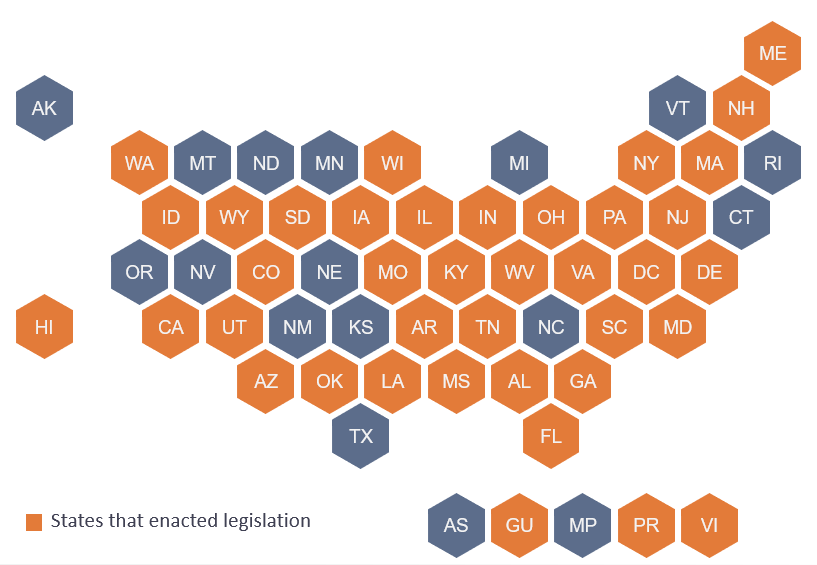
Administration
At least 14 states enacted legislation related to EMS administration, including declaring EMS as an essential service that state, county or municipal governments must provide to residents. Criteria vary by state, but such measures may establish minimum EMS requirements across a state (such as minimum number of ambulances per county), provide flexibility to organize and finance EMS systems at the local level or provide resources to support EMS system improvement.
As of December, at least 13 states had designated EMS as essential in statute. New to the list are South Carolina and Maine. South Carolina (HB 4601) designated ambulances services as essential and required that each county governing body ensure that at least one licensed ambulance service is operating within the county. In addition to establishing EMS as an essential service, Maine (HB 1474) established a commission to study EMS in the state. The commission’s final report identified a nearly $70 million gap between the cost of providing services and current subsidies.
Funding
One of the primary funding challenges is that health care reimbursements—particularly from Medicare or Medicaid—do not cover the total cost of providing EMS care. EMS agencies often are not reimbursed for services unless a patient is transported to a hospital. At least 22 states enacted legislation in 2022 addressing these challenges.
Some states, including Idaho and Maryland, have increased supplemental Medicaid reimbursements to cover uncompensated costs. Idaho (SB 1283) supplemented reimbursements to publicly owned ambulance agencies for providing emergency ground transportation services to Medicaid recipients. Maryland (SB 295) expanded the services for which Medicaid is required to reimburse EMS providers and required the state health department to increase reimbursements by each fiscal year.
Rules and Regulations
States have the authority to regulate EMS delivery, including rules and regulations on data collection, air ambulance services, emergency services for children and liability protections for EMS clinicians. At least three states—Indiana (SB 185), Kentucky (HB 442) and Virginia (HB 16)—enacted bills setting requirements for the installation of newborn safety devices (or devices permitting a parent to anonymously place a newborn with the intent to surrender custody of the child) by ground ambulance and other EMS providers.
Systems of Care
Systems of care provide coordinated efforts in defined geographic areas for the delivery of health services such as EMS and trauma, stroke and acute cardiac care. Systems of care allow EMS clinicians to collaborate with hospital partners to improve patient outcomes through rapid diagnosis, stabilization and transport to an appropriate facility. At least 10 states enacted bills related to systems of care in 2022. Louisiana (SB 411) expanded the focus of the state emergency response network to address stroke and acute cardiac response alongside trauma. Massachusetts (HB 5050) required the state health department to provide quality improvement measures that align with stroke consensus metrics and expand the statewide registry that compiles information and statistics on stroke care.
Workforce
Communities across the country—but particularly in rural areas—are facing challenges in recruiting and retaining EMS clinicians. Research suggests that a decline in volunteerism in part may account for EMS workforce shortages nationally.
In 2022, states enacted legislation to improve the recruitment and retention of volunteer first responders through tax credits, employee benefits and additional workplace training opportunities. Delaware (SB 189) increased the tax credit for active members of volunteer fire, ambulance and rescue service companies from $500 to $1,000. And Utah (HB 289) authorized volunteer EMS personnel working for a local government entity to participate in the Public Employee’s Benefit and Insurance Program.
NCSL would like to acknowledge the National Highway Traffic Safety Administration for supporting this database.
Kelsie George is a policy specialist in NCSL’s Health Program.