Mental health conditions and disorders among children and adolescents have been on the rise for years. And while the impacts of COVID-19 on child and adolescent mental health are not fully known, increased reports of anxiety, depression and emotional and physical abuse have experts calling on adults, communities and leaders to prioritize youth health through preventive intervention and treatment.
Learning to identify and treat mental health warning signs and symptoms can increase the ability of children and adolescents to develop coping and resiliency skills that help them learn, behave and handle their emotions. These skills are essential to healthy social development and help ensure children have a positive quality of life into adulthood.
Because children and adolescents are still developing, they may express and articulate their distress differently than adults. Health care professionals use clinical guidelines, while parents, adults and peers may need to look for other cues. More apparent symptoms are generally behavioral and can appear through changes in school performance and increased frequency of nightmares, disobedience, aggression and temper tantrums. For adolescents, increased thoughts of sadness, hopelessness and suicidal ideation can be common symptoms. Commonly diagnosed children’s mental disorders include:
- Anxiety.
- Depression.
- Attention deficit/hyperactive disorder (ADHD).
- Oppositional defiant disorder.
- Conduct disorder.
- Obsessive-compulsive disorder.
- Post-traumatic stress disorder.
- Tourette syndrome.
The American Academy of Child and Adolescent Psychiatry recommends health care providers routinely screen children for behavioral and mental health concerns. Early identification of symptoms and connection to child therapy or family therapy, or both, can reduce a child’s risk of persistent or increased mental health challenges. Adolescents who experience difficulties with anxiety or depression may benefit from cognitive behavioral therapy, which allows older children to work on new ways of thinking and reacting.
Rising Rates of Mental and Behavioral Health Disorders
Newly released public health data from the Centers for Disease Control and Prevention shows rising rates of mental, emotional and behavioral disorders among children and adolescents. From 2013-2019, ADHD and anxiety disorders were among the most common diagnoses for children ages 3-17, with approximately 1 in 11 children diagnosed. Depression and suicide were rated as high risk for adolescents ages 12-17. During the same period, 1 in 5 adolescents experienced a major depressive episode or seriously considered suicide.
The 2019 Youth Risk Behavior Survey reveals suicide attempts increased overall and that those most at risk include females, non-Hispanic whites, non-Hispanic Blacks, 12th graders and sexual minorities, especially LGBTQ+ youth. Suicide is the second-leading cause of death among youth ages 14-18. Adolescents who struggle with suicidal ideation or who attempt suicide usually do so because of a combination of individual, community and societal stressors. Suicide is often associated with people who have experienced toxic stress, which is often caused by adverse childhood experiences including abuse and neglect, bullying, peer violence and dating or sexual violence.
Mental health disorders have been linked to substance misuse and increased risky behaviors among adolescents and young adults, especially when use is started earlier in life. Data released in 2022 shows at least 1 in 8 young adults have reported using illicit substances within the last year. The Illicit use of alcohol, cannabis, opioids and prescription drugs is reported most among adolescents and young adults. The misuse of stimulants, opioids and depressants can have harmful effects on the developing adolescent brain and body.
A public health approach to behavioral health challenges can allow for increased and earlier identification of risk factors, increased awareness of mental health disorders, elimination or reduction of stigma and health inequities, and improved access to treatment for entire communities. Through preventive intervention and treatment, along with system collaboration and alignment, policymakers can be better equipped to make decisions without duplicating efforts and reduce overall health care system costs.
State Actions: Expanding Awareness and Access
Many states have enacted legislation to increase awareness of youth mental health needs, address adverse childhood experiences and improve access to mental health treatment. In 2021, Kentucky designated an official state mental health flag to encourage residents, government agencies, schools, businesses, and public and private institutions to commit to increasing awareness and understanding of mental health. Maryland called for the state to add questions on adverse childhood experiences, or positive childhood experiences, to its administration of the CDC’s Youth Risk Behavior Survey. Colorado created the I Matter program, which connects anyone 18 or younger with a therapist for up to three free, virtual or in-person counseling sessions. Adolescents as young as 12 can access services without a parent or guardian.
Schools also continue to be an important access point for children and adolescents seeking mental and behavioral health care services. Rhode Island’s 2021 Nathan Bruno and Jason Flatt Act requires the training of teachers, students and school personnel on suicide awareness and prevention efforts. Alabama passed legislation to require the state department of education to develop a program to address the mental health of “Tier II students,” who are considered at-risk for developing inadequate social-behavioral skills, such as ADHD or anger-management issues. Washington established an office within the health department to award grants and coordinate with other agencies and entities to provide support, training and technical assistance to school-based health centers. In its research, the Legislature highlighted increasing health and academic disparities for students of color during COVID-19 and acknowledged “school-based health centers’ role in advancing equity by providing health care access and support at schools.”
States With Expanded Medicaid School Coverage
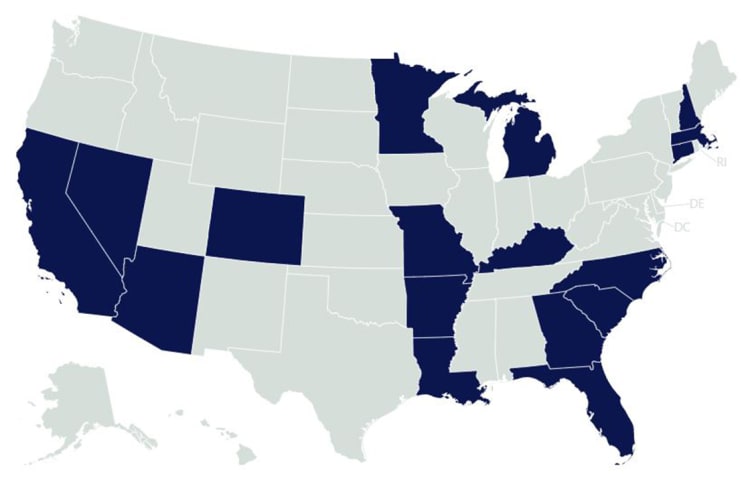
Source: Healthy Students, Promising Futures: School Medicaid Programs
Federal Funding and Support
Approximately 34.8% of children ages 0-18 were covered under Medicaid, according to a 2020 Kaiser Family Foundation report. Through the Early and Periodic Screening, Diagnostic and Treatment benefit, Medicaid can play a role in connecting children and adolescents to preventive health care, including mental health and developmental services. Medicaid can also support sustainable funding for school mental and behavioral health services through federal reimbursement. At least 17 states have expanded Medicaid coverage of services in schools as of December 2021.
Medicaid can also support the use of Screening, Brief Intervention and Referral to Treatment, an early intervention practice for people who have a substance use disorder or for those at risk of developing a disorder. Experts have developed a youth version of the approach for children and adolescents 9-18 who may be at risk of substance use or misuse.
In 2021, the Department of Health and Human Services awarded $10.7 million from the American Rescue Plan to expand pediatric mental health care access, and in March, the HHS and the Office of Minority Health announced nearly $35 million in funding opportunities to strengthen and expand community mental health services and suicide prevention programs for children and young adults.
Tammy Jo Hill is a senior policy specialist in NCSL’s Health Program.
This project is supported by the Centers for Disease Control and Prevention of the U.S. Department of Health and Human Services as part of a financial assistance award totaling $200,000 with 100% funded by the CDC/HHS. The contents are those of the author(s) and do not necessarily represent the official views of, nor an endorsement by, the CDC/HHS or the U.S. government.